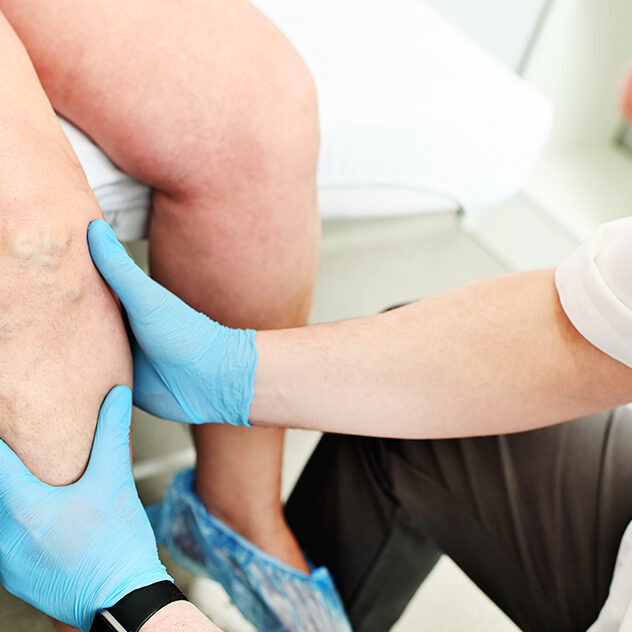
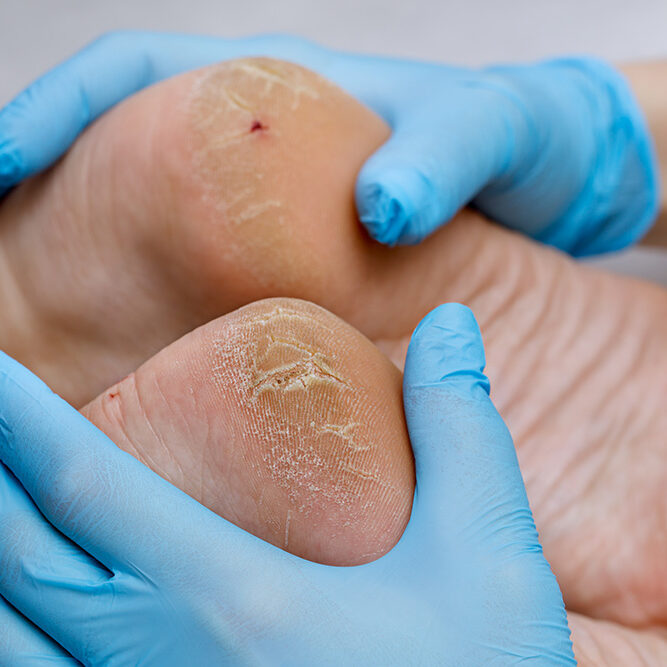
What Is Peripheral Venous Disease?
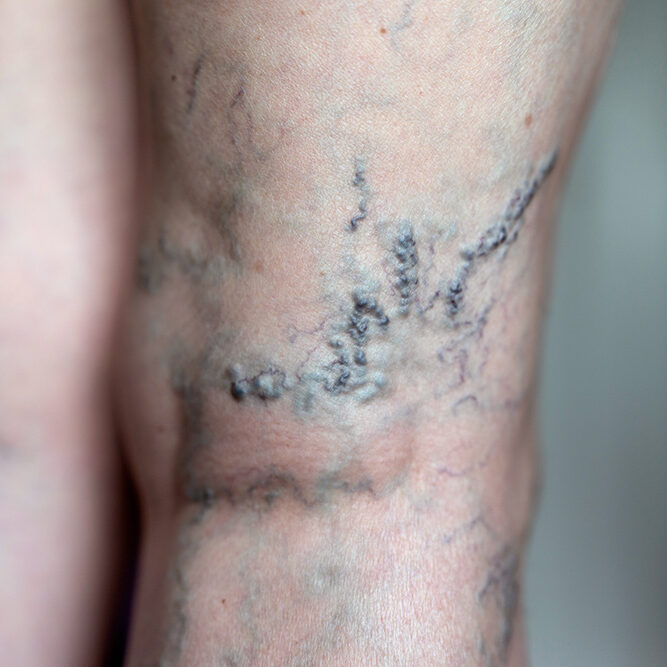
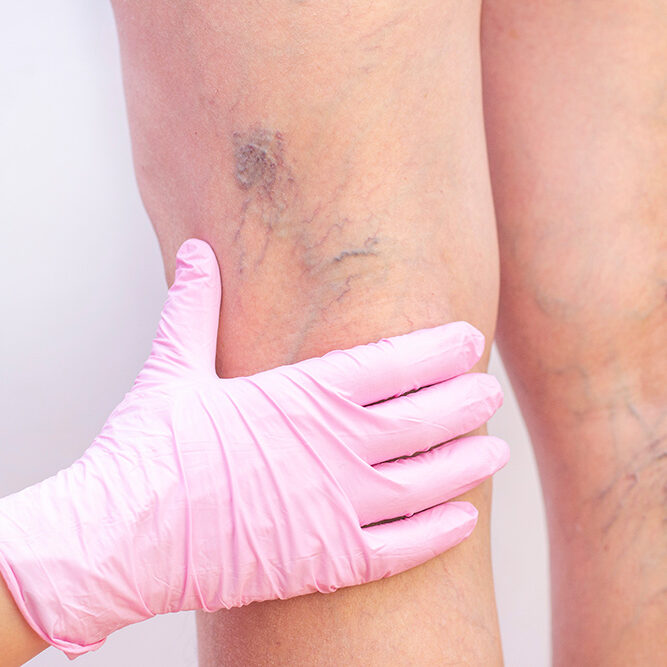
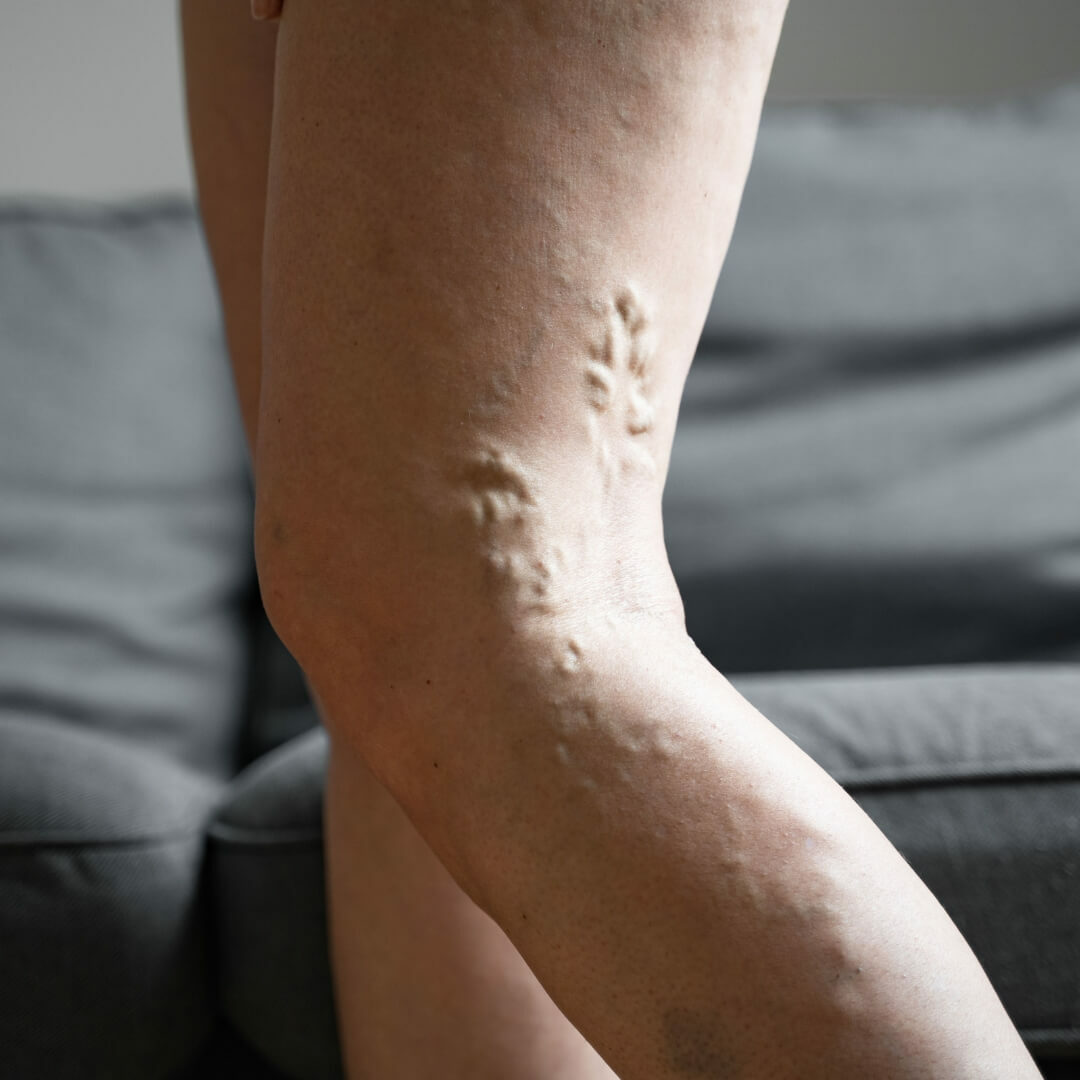
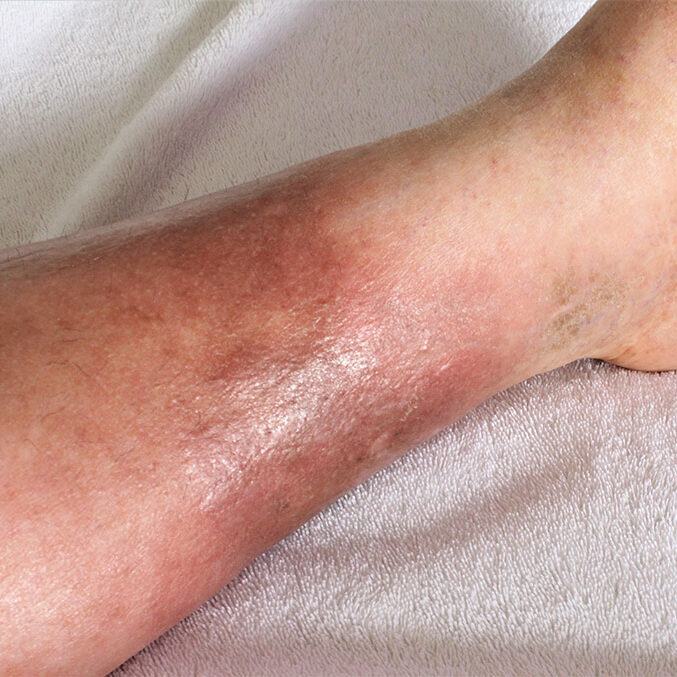
Peripheral Venous Disease (PVD) is a condition impacting blood vessels beyond the heart and brain, predominantly in the legs and arms. It occurs when these vessels narrow or become insufficient, impeding the smooth blood flow back to the heart. Disruption of this flow, due to vessel narrowing or blockage, can result in symptoms like heaviness, fatigue, swelling, discomfort, varicose veins, and difficult-to-heal ulcers. The most prevalent form of PVD is chronic venous insufficiency (CVI), where vein valves that return blood to the heart are damaged or weakened, causing blood to flow backward and accumulate in the veins. This leads to symptoms such as leg pain, swelling, varicose veins, skin changes, and ulcers. Recognized as a medical condition by Medicare, Medicaid, and private insurance carriers, vein disease affects over 30 million people in the United States.
As vascular surgeons, we are equipped with the expertise to effectively treat PVD and its complications, benefiting our community immensely. We understand the significance of addressing PVD to prevent complications like chronic venous insufficiency, ulcers, and slow-healing wounds. With our specialized knowledge and advanced treatments, we are proud to play a pivotal role in meeting the growing healthcare needs of our community.
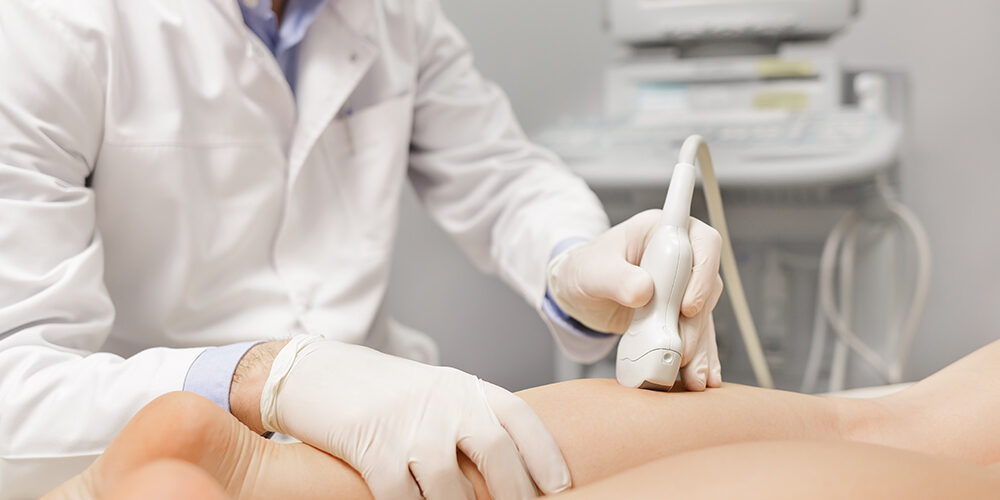
Symptoms of Peripheral Venous Disease (PVD) We Commonly Treat
Treating Peripheral Venous Disease
Diagnosing Peripheral Venous Disease (PVD) necessitates a meticulous approach, considering its varied clinical manifestations. Patients commonly present with symptoms including swelling, discomfort, heaviness, and visibly dilated veins. At NEPA Vascular, we employ state-of-the-art diagnostic modalities, prominently ultrasound imaging, to accurately assess the extent and severity of PVD. Through a thorough evaluation of symptoms coupled with a detailed medical history analysis, we develop a customized treatment plan specific to each patient, ensuring precision in identifying and addressing the condition effectively. The primary objectives of managing PVD are to manage its symptoms and prevent the disease from advancing, thus minimizing the likelihood of experiencing complications like heart attack or stroke. At NEPA Vascular, we pride ourselves on offering a comprehensive range of treatments to combat PVD and its associated complications. Our approach involves a combination of cutting-edge medical interventions tailored to individual patient needs and can include the following modalities.
Venaseal Treatment
Venaseal Treatment represents a cutting-edge approach to tackling varicose veins, utilizing advanced techniques to deliver optimal results. This innovative procedure involves the application of medical-grade adhesive to seal off problematic varicose veins. Unlike traditional methods, such as thermal or sclerosant treatments, Venaseal Treatment offers a non-thermal, non-sclerosant alternative, enhancing patient comfort and expediting the recovery process. By effectively eliminating venous reflux, this procedure not only alleviates distressing symptoms but also promotes the long-term health and functionality of the veins. Its precision and efficacy make it a preferred choice for individuals seeking lasting relief from varicose vein-related issues.
Endovenous Laser Treatment (EVLT)
Endovenous Laser Ablation (EVLT) stands as a cornerstone in the modern approach to treating varicose veins, offering a highly effective and minimally invasive solution. During the procedure, a thin fiber-optic probe is inserted into the affected vein through a small incision, typically made near the knee or ankle, guided by ultrasound imaging. Once in place, laser energy is emitted through the probe, precisely targeting and heating the walls of the faulty vein. This controlled thermal energy effectively seals off the vein, rerouting blood flow to healthier vessels nearby. By addressing the root cause of varicose veins, EVLT not only relieves symptoms but also visibly diminishes their appearance over time. Patients often appreciate the procedure's minimal discomfort and short recovery period, enabling them to return to their daily routines with ease. EVLT's combination of precision, efficacy, and patient satisfaction has made it a preferred choice among healthcare providers and individuals seeking lasting relief from varicose vein issues.
Deep Venous Treatment
Deep Venous Treatment encompasses a range of minimally invasive procedures aimed at addressing conditions that affect the deep veins of the body. One common approach involves the use of balloon-like devices or stents to restore proper blood flow in narrowed or obstructed veins. During the procedure, a catheter equipped with a deflated balloon or a collapsible stent is carefully guided to the site of the blockage using imaging techniques such as fluoroscopy or ultrasound. Once positioned, the balloon or stent is inflated or expanded, gently widening the narrowed vessel and improving blood circulation. This intervention not only alleviates symptoms associated with reduced blood flow, such as swelling and discomfort, but also helps prevent complications like deep vein thrombosis (DVT) or venous ulcers. Deep Venous Treatment is valued for its minimally invasive nature, which often translates to shorter recovery times and reduced risk of complications compared to traditional surgical interventions. By restoring proper venous blood flow, these procedures play a crucial role in improving the overall health and function of the circulatory system.
Take Control of PVD with NEPA Vascular
At NEPA Vascular, we understand the complexities and potential complications that can arise from peripheral vascular disease (PVD) if left untreated. From reduced mobility to more severe conditions like ulcers and amputation, the impact on your quality of life can be significant. That's why our team of experienced vascular specialists is dedicated to providing personalized care and innovative treatments to effectively manage PVD and its associated risks. Don't wait until it's too late. Take control of your vascular health today and schedule a consultation with NEPA Vascular. Let us help you regain comfort, mobility, and peace of mind. Contact us now to take the first step towards a healthier future.